Influenza pandemic
| Influenza (Flu) |
|---|
 |
| Types |
| Avian (A/H5N1 subtype) · Canine Equine · Swine (A/H1N1 subtype) |
| Vaccines |
| 2009 pandemic (Pandemrix) ACAM-FLU-A · Fluzone · Influvac Live attenuated (FluMist) · Optaflu |
| Treatment |
| Amantadine · Arbidol · Laninamivir Oseltamivir · Peramivir · Rimantadine Vitamin D · Zanamivir |
| Pandemics |
| 2009 · 1968–1969 Hong Kong · 1918 |
| Outbreaks |
| 2008 West Bengal 2007 Bernard Matthews H5N1 2007 Australian equine 2006 H5N1 India · 1976 swine flu |
| See also |
| Flu season · Influenza evolution Influenza research Influenza-like illness |

An influenza pandemic is an epidemic of an influenza virus that spreads on a worldwide scale and infects a large proportion of the human population. In contrast to the regular seasonal epidemics of influenza, these pandemics occur irregularly, with the 1918 Spanish flu the most serious pandemic in recent history. Pandemics can cause high levels of mortality, with the Spanish influenza estimated as being responsible for the deaths of over 50 million people. There have been about three influenza pandemics in each century for the last 300 years. The most recent ones were the Asian Flu in 1957 and the Hong Kong Flu in 1968.[1]
Influenza pandemics occur when a new strain of the influenza virus is transmitted to humans from another animal species. Species that are thought to be important in the emergence of new human strains are pigs, chickens and ducks. These novel strains are unaffected by any immunity people may have to older strains of human influenza and can therefore spread extremely rapidly and infect very large numbers of people. Influenza A viruses can occasionally be transmitted from wild birds to other species causing outbreaks in domestic poultry and may give rise to human influenza pandemics.[2][3]
The World Health Organization (WHO) has produced a six-stage classification that describes the process by which a novel influenza virus moves from the first few infections in humans through to a pandemic. This starts with the virus mostly infecting animals, with a few cases where animals infect people, then moves through the stage where the virus begins to spread directly between people, and ends with a pandemic when infections from the new virus have spread worldwide.[4]
One strain of virus that may produce a pandemic in the future is a highly pathogenic variation of the H5N1 subtype of Influenza A virus. On 11 June 2009, a new strain of H1N1 influenza was declared to be a global pandemic (Stage 6) by the World Health Organization after evidence of spreading in the southern hemisphere.[5] November 8, 2009 worldwide update by the U.N.'s World Health Organization (WHO) states that "206 countries and overseas territories/communities have officially reported over 503,536 laboratory confirmed cases of the influenza pandemic H1N1 infection, including 6,250 deaths."[5]
Influenza
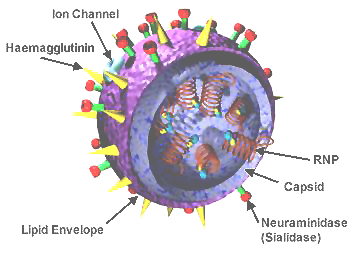
Influenza, commonly known as flu, is an infectious disease of birds and mammals caused by an RNA virus of the family Orthomyxoviridae (the influenza viruses). In humans, common symptoms of influenza infection are fever, sore throat, muscle pains, severe headache, coughing, and weakness and fatigue.[6] In more serious cases, influenza causes pneumonia, which can be fatal, particularly in young children and the elderly. While sometimes confused with the common cold, influenza is a much more severe disease and is caused by a different type of virus.[7] Although nausea and vomiting can be produced, especially in children,[6] these symptoms are more characteristic of the unrelated gastroenteritis, which is sometimes called "stomach flu" or "24-hour flu."[8]
Typically, influenza is transmitted from infected mammals through the air by coughs or sneezes, creating aerosols containing the virus, and from infected birds through their droppings. Influenza can also be transmitted by saliva, nasal secretions, feces and blood. Healthy individuals can become infected if they breathe in a virus-laden aerosol directly, or if they touch their eyes, nose or mouth after touching any of the aforementioned bodily fluids (or surfaces contaminated with those fluids). Flu viruses can remain infectious for about one week at human body temperature, over 30 days at 0 °C (32 °F), and indefinitely at very low temperatures (such as lakes in northeast Siberia). Most influenza strains can be inactivated easily by disinfectants and detergents.[9][10][11]
Flu spreads around the world in seasonal epidemics. Three influenza pandemics occurred in the 20th century and killed tens of millions of people, with each of these pandemics being caused by the appearance of a new strain of the virus in humans. Often, these new strains result from the spread of an existing flu virus to humans from other animal species. When it first killed humans in Asia in the 1990s, a deadly avian strain of H5N1 posed a great risk for a new influenza pandemic; however, this virus did not mutate to spread easily between people.[12]
Vaccinations against influenza are most commonly given to high-risk humans in industrialized countries[13] and to farmed poultry.[14] The most common human vaccine is the trivalent influenza vaccine that contains purified and inactivated material from three viral strains. Typically this vaccine includes material from two influenza A virus subtypes and one influenza B virus strain.[15] A vaccine formulated for one year may be ineffective in the following year, since the influenza virus changes rapidly over time and different strains become dominant. Antiviral drugs can be used to treat influenza, with neuraminidase inhibitors being particularly effective.
Variants and subtypes of Influenzavirus A
Variants of Influenzavirus A are identified and named according to the isolate that they are like and thus are presumed to share lineage (example Fujian flu virus like); according to their typical host (example Human flu virus); according to their subtype (example H3N2); and according to their deadliness (example LP). So a flu from a virus similar to the isolate A/Fujian/411/2002(H3N2) is called Fujian flu, human flu, and H3N2 flu.
Variants are sometimes named according to the species (host) the strain is endemic in or adapted to. Some variants named using this convention are:[17]
Avian variants have also sometimes been named according to their deadliness in poultry, especially chickens:
- Low Pathogenic Avian Influenza (LPAI)
- Highly Pathogenic Avian Influenza (HPAI), also called: deadly flu or death flu
The Influenza A virus subtypes are labeled according to an H number (for hemagglutinin) and an N number (for neuraminidase). Each subtype virus has mutated into a variety of strains with differing pathogenic profiles; some pathogenic to one species but not others, some pathogenic to multiple species. Most known strains are extinct strains. For example, the annual flu subtype H3N2 no longer contains the strain that caused the Hong Kong Flu.[18]
Influenza A viruses are negative sense, single-stranded, segmented RNA viruses. "There are 16 different HA antigens (H1 to H16) and nine different NA antigens (N1 to N9) for influenza A. Until recently, 15 HA types had been recognized, but a new type (H16) was isolated from black-headed gulls caught in Sweden and the Netherlands in 1999 and reported in the literature in 2005."[19]
Nature of a flu pandemic
Some pandemics are relatively minor such as the one in 1957 called "Asian flu" (1 - 4 million dead, depending on source). Others have a higher Pandemic Severity Index whose severity warrants more comprehensive social isolation measures.[20]
The 1918 pandemic killed tens of millions and sickened hundreds of millions; the loss of this many people in the population caused upheaval and psychological damage to many people.[21] There were not enough doctors, hospital rooms, or medical supplies for the living as they contacted the disease. Dead bodies were often left unburied as few people were available to deal with them. There can be great social disruption as well as a sense of fear. Efforts to deal with pandemics can leave a great deal to be desired because of human selfishness, lack of trust, illegal behavior, and ignorance. For example in the 1918 pandemic: "This horrific disconnect between reassurances and reality destroyed the credibility of those in authority. People felt they had no one to turn to, no one to rely on, no one to trust."[22]
A letter from a physician at one U.S. Army camp in the 1918 pandemic said:
- It is only a matter of a few hours then until death comes [...]. It is horrible. One can stand it to see one, two or twenty men die, but to see these poor devils dropping like flies [...]. We have been averaging about 100 deaths per day [...]. Pneumonia means in about all cases death [...]. We have lost an outrageous number of Nurses and Drs. It takes special trains to carry away the dead. For several days there were no coffins and the bodies piled up something fierce [...].[23]
Wave nature
Flu pandemics typically come in waves. The 1889–1890 and 1918–1919 flu pandemics each came in three or four waves of increasing lethality.[24] But within a wave, mortality was greater at the beginning of the wave.[25]
Variable mortality
Mortality varies widely in a pandemic. In the 1918 pandemic:
- In U.S. Army camps where reasonably reliable statistics were kept, case mortality often exceeded 5 percent, and in some circumstances exceeded 10 percent. In the British Army in India, case mortality for white troops was 9.6 percent, for Indian troops 21.9 percent. In isolated human populations, the virus killed at even higher rates. In the Fiji islands, it killed 14 percent of the entire population in 16 days. In Labrador and Alaska, it killed at least one-third of the entire native population.[26]
Notable influenza pandemics
| Name of pandemic | Date | Deaths | Subtype involved |
|---|---|---|---|
| Asiatic (Russian) Flu | 1889–90 | 1 million | possibly H2N2 |
| Spanish Flu | 1918–20 | 50 million | H1N1 |
| Asian Flu | 1957–58 | 1.5 to 2 million | H2N2 |
| Hong Kong Flu | 1968–69 | 1 million | H3N2 |
| Swine Flu | As of January 24th, 2010 | 14,711[6] | novel H1N1 |
Spanish Flu (1918–1920)
The 1918 flu pandemic, commonly referred to as the Spanish flu, was a category 5 influenza pandemic caused by an unusually severe and deadly Influenza A virus strain of subtype H1N1.
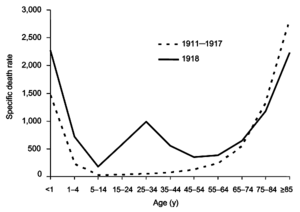
The difference between the influenza mortality age-distributions of the 1918 epidemic and normal epidemics. Deaths per 100,000 persons in each age group, United States, for the interpandemic years 1911–1917 (dashed line) and the pandemic year 1918 (solid line).[28]
The Spanish flu pandemic lasted from 1918 to 1919, although Price-Smith's data suggest it may have begun in Austria in the Spring of 1917.[29] Older estimates say it killed 40–50 million people[30] while current estimates say 50 million to 100 million people worldwide were killed.[24] This pandemic has been described as "the greatest medical holocaust in history" and may have killed as many people as the Black Death,[31] although the Black Death is estimated to have killed over a fifth of the world's population at the time,[32] a significantly higher proportion. This huge death toll was caused by an extremely high infection rate of up to 50% and the extreme severity of the symptoms, suspected to be caused by cytokine storms.[30] Indeed, symptoms in 1918 were so unusual that initially influenza was misdiagnosed as dengue, cholera, or typhoid. One observer wrote, "One of the most striking of the complications was hemorrhage from mucous membranes, especially from the nose, stomach, and intestine. Bleeding from the ears and petechial hemorrhages in the skin also occurred."[24] The majority of deaths were from bacterial pneumonia, a secondary infection caused by influenza, but the virus also killed people directly, causing massive hemorrhages and edema in the lung.[28]
The Spanish flu pandemic was truly global, spreading even to the Arctic and remote Pacific islands. The unusually severe disease killed between 2 and 20% of those infected, as opposed to the more usual flu epidemic mortality rate of 0.1%.[24][28] Another unusual feature of this pandemic was that it mostly killed young adults, with 99% of pandemic influenza deaths occurring in people under 65, and more than half in young adults 20 to 40 years old.[33] This is unusual since influenza is normally most deadly to the very young (under age 2) and the very old (over age 70). The total mortality of the 1918–1919 pandemic is not known, but it is estimated that up to 1% of the world's population was killed. As many as 25 million may have been killed in the first 25 weeks; in contrast, HIV/AIDS has killed 25 million in its first 25 years.[24]
The Manchester Influenza Epidemic of 1937
The Epidemic that never escalated to Pandemic This is an example of an interwar epidemic that public health controls did not allow to develop into a full blown pandemic because of what was already known from 1918, as well as employing very strict patient, contact and family isolation. In 1937 there were 620 claims for sickness benefits made to various insurance companies.[34]
Asian Flu (1957–1958)
The "Asian Flu" was a category 2 flu pandemic outbreak of avian influenza that originated in China in early 1956 lasting until 1958. It originated from mutation in wild ducks combining with a pre-existing human strain.[35] The virus was first identified in Guizhou.[36] It spread to Singapore in February 1957, reached Hong Kong by April, and US by June. Death toll in the US was approximately 69,800.[35] The elderly were particularly vulnerable.[37] Estimates of worldwide deaths vary widely depending on source, ranging from 1 million to 4 million.
Hong Kong Flu (1968–1969)
The Hong Kong Flu was a category 2 flu pandemic caused by a strain of H3N2 descended from H2N2 by antigenic shift, in which genes from multiple subtypes reassorted to form a new virus. The Hong Kong Flu pandemic of 1968 and 1969 killed an estimated one million people worldwide.[38][39][40] Those over 65 had the greatest death rates[37]. In the US, there were about 33,800 deaths.[41]
2009 Flu Pandemic (Since 2009)
In March-April 2009, an epidemic of influenza-like illness of unknown causation occurred in Mexico. On April 24, 2009, following the isolation of an A/H1N1 influenza in 7 ill patients in the southwest US. The WHO issued a statement on the outbreak of "influenza like illness" in the confirmed cases of A/H1N1 influenza had been reported in Mexico, and that 20 confirmed cases of the disease had been reported in the US.The next day, the number of confirmed cases rose to 40 in the US, 26 in Mexico, 6 in Canada, and 1 in Spain.The disease spread rapidly through the rest the spring, and by May 3, 787 confirmed cases of the disease had been reported worldwide.[42] On June 11, 2009, the ongoing outbreak of Influenza A/H1N1, commonly referred to as "swine flu", was officially declared by the WHO to be the first influenza pandemic of the 21st century and a new strain of Influenza A virus subtype H1N1 first identified in April 2009. .[43] It is thought to be a mutation (reassortment) of four known strains of influenza A virus subtype H1N1: one endemic in humans, one endemic in birds, and two endemic in pigs (swine).[44]
In November 1, 2009 a worldwide update by the U.N.'s World Health Organization (WHO) stated that "199 countries and overseas territories/communities have officially reported a total of over 482,300 laboratory confirmed cases of the influenza pandemic H1N1 infection, that included 6,071 deaths."[45]
H5N1
 |
|
Influenza A virus subtype H5N1, also known as A(H5N1) or simply H5N1, is a subtype of the Influenza A virus which can cause illness in humans and many other animal species.[46] A bird-adapted strain of H5N1, called HPAI A(H5N1) for "highly pathogenic avian influenza virus of type A of subtype H5N1", is the causative agent of H5N1 flu, commonly known as "avian influenza" or "bird flu". It is endemic in many bird populations, especially in Southeast Asia. One strain of HPAI A(H5N1) is spreading globally after first appearing in Asia. It is epizootic (an epidemic in nonhumans) and panzootic (affecting animals of many species, especially over a wide area), killing tens of millions of birds and spurring the culling of hundreds of millions of others to stem its spread. Most mentions of "bird flu" and H5N1 in the media refer to this strain.[47]
HPAI A(H5N1) is an avian disease. There is no evidence of efficient human-to-human transmission or of airborne transmission of HPAI A(H5N1) to humans. In almost all cases, those infected with H5N1 had extensive physical contact with infected birds. Still, around 60% of humans known to have been infected with the current Asian strain of HPAI A(H5N1) have died from it, and H5N1 may mutate or reassort into a strain capable of efficient human-to-human transmission.[48][49][50][51][52][53][54]
In 2003, world-renowned virologist Robert G. Webster published an article titled "The world is teetering on the edge of a pandemic that could kill a large fraction of the human population" in American Scientist. He called for adequate resources to fight what he sees as a major world threat to possibly billions of lives.[55] On September 29, 2005, David Nabarro, the newly-appointed Senior United Nations System Coordinator for Avian and Human Influenza, warned the world that an outbreak of avian influenza could kill anywhere between 5 million and 150 million people.[56] Experts have identified key events (creating new clades, infecting new species, spreading to new areas) marking the progression of an avian flu virus towards becoming pandemic, and many of those key events have occurred more rapidly than expected.
Due to the high lethality and virulence of HPAI A(H5N1), its endemic presence, its increasingly large host reservoir, and its significant ongoing mutations, the H5N1 virus is the world's largest current pandemic threat, and billions of dollars are being spent researching H5N1 and preparing for a potential influenza pandemic.[57] At least 12 companies and 17 governments are developing pre-pandemic influenza vaccines in 28 different clinical trials that, if successful, could turn a deadly pandemic infection into a nondeadly one. Full-scale production of a vaccine that could prevent any illness at all from the strain would require at least three months after the virus's emergence to begin, but it is hoped that vaccine production could increase until one billion doses were produced by one year after the initial identification of the virus.[58]
H5N1 may cause more than one influenza pandemic as it is expected to continue mutating in birds regardless of whether humans develop herd immunity to a future pandemic strain.[59] Influenza pandemics from its genetic offspring may include influenza A virus subtypes other than H5N1.[60] While genetic analysis of the H5N1 virus shows that influenza pandemics from its genetic offspring can easily be far more lethal than the Spanish Flu pandemic,[61] planning for a future influenza pandemic is based on what can be done and there is no higher Pandemic Severity Index level than a Category 5 pandemic which, roughly speaking, is any pandemic as bad the Spanish flu or worse; and for which all intervention measures are to be used.[20]
H5N1 is just one of the many subtypes of the species Influenza A virus. Any one of them can combine with each other or with different variant genotypes within its own subtype creating new variants, any one of which could become a pandemic strain. We know enough about the genetics to know what strains to fear most (example: only H5 and H7 subtypes are "highly pathogenic") and we know what genetic factors make a flu virus a human virus (i.e. easily passed human to human); so we know H5N1 is the biggest pandemic threat of all the strains in circulation and we know it is only a few antigenic shift mutations or antigenic drift mutations from being an avian influenza virus to being a human flu virus. If it does this it may or may not still be in the H5N1 subtype. Both the drift and the shift can happen in any infected animal and then be passed to a human and spread like wildfire. Possible shift scenarios include the shift occurring in humans, pigs, or cats. To acquire the needed mutation through drift, it simply has to continue being an epidemic in birds long enough for the mutations to occur and then be passed to a human.
Other pandemic threat subtypes
"Human influenza virus" usually refers to those subtypes that spread widely among humans. H1N1, H1N2, and H3N2 are the only known Influenza A virus subtypes currently circulating among humans.[62]
Genetic factors in distinguishing between "human flu viruses" and "avian influenza viruses" include:
- PB2: (RNA polymerase): Amino acid (or residue) position 627 in the PB2 protein encoded by the PB2 RNA gene. Until H5N1, all known avian influenza viruses had a Glu at position 627, while all human influenza viruses had a lysine.
- HA: (hemagglutinin): Avian influenza HA bind alpha 2-3 sialic acid receptors while human influenza HA bind alpha 2-6 sialic acid receptors. Swine influenza viruses have the ability to bind both types of sialic acid receptors.
"About 52 key genetic changes distinguish avian influenza strains from those that spread easily among people, according to researchers in Taiwan, who analyzed the genes of more than 400 A type flu viruses."[63] "How many mutations would make an avian virus capable of infecting humans efficiently, or how many mutations would render an influenza virus a pandemic strain, is difficult to predict. We have examined sequences from the 1918 strain, which is the only pandemic influenza virus that could be entirely derived from avian strains. Of the 52 species-associated positions, 16 have residues typical for human strains; the others remained as avian signatures. The result supports the hypothesis that the 1918 pandemic virus is more closely related to the avian influenza A virus than are other human influenza viruses."[64]
Highly pathogenic H5N1 avian influenza kills 50% of humans that catch it. In one case, a boy with H5N1 experienced diarrhea followed rapidly by a coma without developing respiratory or flu-like symptoms.[65]
The Influenza A virus subtypes that have been confirmed in humans, ordered by the number of known human pandemic deaths, are:
- H1N1 caused "Spanish Flu" and the 2009 swine flu outbreak (novel H1N1)
- H2N2 caused "Asian Flu"
- H3N2 caused "Hong Kong Flu"
- H5N1 is "bird flu", endemic in avians
- H7N7 has unusual zoonotic potential
- H1N2 is currently endemic in humans and pigs
- H9N2, H7N2, H7N3, H10N7
- H1N1
- H1N1 is currently endemic in both human and pig populations. A variant of H1N1 was responsible for the Spanish flu pandemic that killed some 50 million to 100 million people worldwide over about a year in 1918 and 1919.[66] Controversy arose in October 2005, after the H1N1 genome was published in the journal, Science. Many fear that this information could be used for bioterrorism.
- "When he compared the 1918 virus with today's human flu viruses, Dr. Taubenberger noticed that it had alterations in just 25 to 30 of the virus's 4,400 amino acids. Those few changes turned a bird virus into a killer that could spread from person to person."[67]
- In mid-April, 2009, an H1N1 variant appeared in Mexico, with its center in Mexico City. By April 26 the variant had spread widely; with cases reported in Canada, the US, New Zealand, the UK, France, Spain and Israel. On 29th April WHO raised the worldwide pandemic phase to 5.[68] On 11 June 2009 the WHO raised the worldwide pandemic phase to 6, which means that the H1N1 swine flu has reached pandemic proportions, with nearly 30,000 confirmed cases worldwide.[69] November 8, 2009 worldwide update by the U.N.'s World Health Organization (WHO) states that "206 countries and overseas territories/communities have officially reported over 503,536 laboratory confirmed cases of the influenza pandemic H1N1 infection, including 6,250 deaths." [7]
1. Microscopic image of the H1N1 virus
2. Microscopic image of the H1N1 virus
- H2N2
- The Asian Flu was a pandemic outbreak of H2N2 avian influenza that originated in China in 1957, spread worldwide that same year during which a influenza vaccine was developed, lasted until 1958 and caused between one and four million deaths.
- H3N2
- H3N2 is currently endemic in both human and pig populations. It evolved from H2N2 by antigenic shift and caused the Hong Kong Flu pandemic of 1968 and 1969 that killed up to 750,000.[70]"An early-onset, severe form of influenza A H3N2 made headlines when it claimed the lives of several children in the United States in late 2003."[71]
- The dominant strain of annual flu in January 2006 is H3N2. Measured resistance to the standard antiviral drugs amantadine and rimantadine in H3N2 has increased from 1% in 1994 to 12% in 2003 to 91% in 2005.[72]
- "[C]ontemporary human H3N2 influenza viruses are now endemic in pigs in southern China and can reassort with avian H5N1 viruses in this intermediate host."[73]
- H7N7
- H7N7 has unusual zoonotic potential. In 2003 in Netherlands 89 people were confirmed to have H7N7 influenza virus infection following an outbreak in poultry on several farms. One death was recorded.
- H1N2
- H1N2 is currently endemic in both human and pig populations. The new H1N2 strain appears to have resulted from the reassortment of the genes of the currently circulating influenza H1N1 and H3N2 subtypes. The hemagglutinin protein of the H1N2 virus is similar to that of the currently circulating H1N1 viruses and the neuraminidase protein is similar to that of the current H3N2 viruses.
Strategies to prevent a flu pandemic
This section contains strategies to prevent a flu pandemic by a Council on Foreign Relations panel.[74]
If influenza remains an animal problem with limited human-to-human transmission it is not a pandemic, though it continues to pose a risk. To prevent the situation from progressing to a pandemic, the following short-term strategies have been put forward:
- Culling and vaccinating livestock
- Vaccinating poultry workers against common flu
- Limiting travel in areas where the virus is found[74]
The rationale for vaccinating poultry workers against common flu is that it reduces the probability of common influenza virus recombining with avian H5N1 virus to form a pandemic strain. Longer term strategies proposed for regions where highly pathogenic H5N1 is endemic in wild birds have included:
- changing local farming practices to increase farm hygiene and reduce contact between livestock and wild birds.
- altering farming practices in regions where animals live in close, often unsanitary quarters with people, and changing the practices of open-air "wet markets" where birds are kept for live sale and slaughtered on-site. A challenge to implementing these measures is widespread poverty, frequently in rural areas, coupled with a reliance upon raising fowl for purposes of subsistence farming or income without measures to prevent propagation of the disease.
- changing local shopping practices from purchase of live fowl to purchase of slaughtered, pre-packaged fowl.
- improving veterinary vaccine availability and cost.[74]
Strategies to slow down a flu pandemic
Vaccines
A vaccine probably would not be available in the initial stages of population infection.[75] A vaccine cannot be developed to protect against a virus which does not exist yet. The Avian Flu virus H5N1 has the potential to mutate into a pandemic strain, but so do other types of flu virus. Once a potential virus is identified and a vaccine is approved, it normally takes five to six months before the vaccine becomes available.[76]
The capability to produce vaccines varies widely from country to country; in fact, only 19 countries are listed as "influenza vaccine manufacturers" according to the World Health Organization.[77] It is estimated that, in a best scenario situation, 750 million doses could be produced each year, whereas it is likely that each individual would need two doses of the vaccine to become immuno-competent. Distribution to and inside countries would probably be problematic.[78] Several countries, however, have well-developed plans for producing large quantities of vaccine. For example, Canadian health authorities say that they are developing the capacity to produce 32 million doses within four months, enough vaccine to inoculate every person in the country.[79]
Another concern is whether countries which do not manufacture vaccines themselves, including those where a pandemic strain is likely to originate, will be able to purchase vaccine to protect their population. Cost considerations aside, they fear that the countries with vaccine-manufacturing capability will reserve production to protect their own populations and not release vaccines to other countries until their own population is protected. Indonesia has refused to share samples of H5N1 strains which have infected and killed its citizens until it receives assurances that it will have access to vaccines produced with those samples. So far, it has not received those assurances.[80] However, in September 2009, The United States and France agreed to make 10 percent of their H1N1 vaccine supply available to other countries through the World Health Organization.[81][82]
There are two serious technical problems associated with the development of a vaccine against H5N1. The first problem is this: seasonal influenza vaccines require a single injection of 15 μg haemagluttinin in order to give protection; H5 seems to evoke only a weak immune response and a large multicentre trial found that two injections of 90 µg H5 given 28 days apart provided protection in only 54% of people (Treanor 2006). Even if it is considered that 54% is an acceptable level of protection, the world is currently capable of producing only 900 million doses at a strength of 15 μg (assuming that all production were immediately converted to manufacturing H5 vaccine); if two injections of 90 μg are needed then this capacity drops to only 70 million (Poland 2006). Trials using adjuvants such as alum, AS03, AS04 or MF59 to try and lower the dose of vaccine are urgently needed. The second problem is this: there are two circulating clades of virus, clade 1 is the virus originally isolated in Vietnam, clade 2 is the virus isolated in Indonesia. Vaccine research has mostly been focused on clade 1 viruses, but the clade 2 virus is antigenically distinct and a clade 1 vaccine will probably not protect against a pandemic caused by clade 2 virus.
Since 2009, most vaccine development efforts have been focused on the current pandemic influenza virus H1N1. As of July 2009, more than 70 known clinical trials are have been completed or are ongoing for pandemic influenza vaccines.[83] In September 2009, the US Food and Drug Administration approved four vaccines against the 2009 H1N1 influenza virus, and expect the initial vaccine lots to be avaialable within the following month.[84]
Anti-viral drugs
Many nations, as well as the World Health Organization, are working to stockpile anti-viral drugs in preparation for a possible pandemic. Oseltamivir (trade name Tamiflu) is the most commonly sought drug, since it is available in pill form. Zanamivir (trade name Relenza) is also considered for use, but it must be inhaled. Other anti-viral drugs are less likely to be effective against pandemic influenza.
Both Tamiflu and Relenza are in short supply, and production capabilities are limited in the medium term. Some doctors say that co-administration of Tamiflu with probenecid could double supplies.[85]
There also is the potential of viruses to evolve drug resistance. Some H5N1-infected persons treated with oseltamivir have developed resistant strains of that virus.
Tamiflu was originally discovered by Gilead Sciences and licensed to Roche for late-phase development and marketing.
Public Response Measures
- Social distancing: By traveling less, working from home or closing schools, there is less opportunity for the virus to spread. Reduce the time spent in crowded settings if possible. And keep your distance (preferably at least 1 metre) from people who show symptoms of influenza-like illness, such as coughing and sneezing.[86]
- Respiratory hygiene: Advise people to cover their coughs and sneezes. If using a tissue, make sure you dispose of it carefully and then clean your hands immediately afterwards. (See "Handwashing Hygiene" below.) If you do not have a tissue handy when you cough or sneeze, cover your mouth as much as possible with the crook of your elbow.[86]
- Handwashing Hygiene: Frequent handwashing with soap and water (or with an alcohol-based hand sanitizer) is very important, especially after coughing or sneezing, and after contact with other people or with potentially contaminated surfaces (such as handrails, shared utensils, etc.)[87]
- Other hygiene: Avoid touching your eyes, nose and mouth as much as possible.[86]
- Masks: No mask can provide a perfect barrier but products that meet or exceed the NIOSH N95 standard recommended by the World Health Organization are thought to provide good protection. WHO recommends that health-care workers wear N95 masks and that patients wear surgical masks (which may prevent respiratory secretions from becoming airborne).[88] Any mask may be useful to remind the wearer not to touch the face. This can reduce infection due to contact with contaminated surfaces, especially in crowded public places where coughing or sneezing people have no way of washing their hands. The mask itself can become contaminated and must be handled as medical waste when removed.
- Risk communication: To encourage the public to comply with strategies to reduce the spread of disease, "communications regarding possible community interventions [such as requiring sick people to stay home from work, closing schools] for pandemic influenza that flow from the federal government to communities and from community leaders to the public not overstate the level of confidence or certainty in the effectiveness of these measures."[89]
The Institute of Medicine has published a number of reports and summaries of workshops on public policy issues related to influenza pandemics. They are collected in Pandemic Influenza: A Guide to Recent Institute of Medicine Studies and Workshops and some strategies from these reports are included in the list above.
Phases
| WHO Pandemic Influenza Phases (2009)[90] | |
|---|---|
| Phase | Description |
| Phase 1 | No animal influenza virus circulating among animals have been reported to cause infection in humans. |
| Phase 2 | An animal influenza virus circulating in domesticated or wild animals is known to have caused infection in humans and is therefore considered a specific potential pandemic threat. |
| Phase 3 | An animal or human-animal influenza reassortant virus has caused sporadic cases or small clusters of disease in people, but has not resulted in human-to-human transmission sufficient to sustain community-level outbreaks. |
| Phase 4 | Human to human transmission of an animal or human-animal influenza reassortant virus able to sustain community-level outbreaks has been verified. |
| Phase 5 | Human-to-human spread of the virus in two or more countries in one WHO region. |
| Phase 6 | In addition to the criteria defined in Phase 5, the same virus spreads from human-to-human in at least one other country in another WHO region. |
| Post peak period | Levels of pandemic influenza in most countries with adequate surveillance have dropped below peak levels. |
| Post pandemic period | Levels of influenza activity have returned to the levels seen for seasonal influenza in most countries with adequate surveillance. |
The World Health Organization (WHO) has developed a global influenza preparedness plan, which defines the stages of a pandemic, outlines WHO's role and makes recommendations for national measures before and during a pandemic.[91]
In the 2009 revision of the phase descriptions, the WHO has retained the use of a six-phase approach for easy incorporation of new recommendations and approaches into existing national preparedness and response plans. The grouping and description of pandemic phases have been revised to make them easier to understand, more precise, and based upon observable phenomena. Phases 1–3 correlate with preparedness, including capacity development and response planning activities, while phases 4–6 clearly signal the need for response and mitigation efforts. Furthermore, periods after the first pandemic wave are elaborated to facilitate post pandemic recovery activities.
The phases are defined below.[92]
In nature, influenza viruses circulate continuously among animals, especially birds. Even though such viruses might theoretically develop into pandemic viruses, in Phase 1 no viruses circulating among animals have been reported to cause infections in humans.
In Phase 2 an animal influenza virus circulating among domesticated or wild animals is known to have caused infection in humans, and is therefore considered a potential pandemic threat.
In Phase 3, an animal or human-animal influenza reassortant virus has caused sporadic cases or small clusters of disease in people, but has not resulted in human-to-human transmission sufficient to sustain community-level outbreaks. Limited human-to-human transmission may occur under some circumstances, for example, when there is close contact between an infected person and an unprotected caregiver. However, limited transmission under such restricted circumstances does not indicate that the virus has gained the level of transmissibility among humans necessary to cause a pandemic.
Phase 4 is characterized by verified human-to-human transmission of an animal or human-animal influenza reassortant virus able to cause "community-level outbreaks". The ability to cause sustained disease outbreaks in a community marks a significant upwards shift in the risk for a pandemic. Any country that suspects or has verified such an event should urgently consult with the WHO so that the situation can be jointly assessed and a decision made by the affected country if implementation of a rapid pandemic containment operation is warranted. Phase 4 indicates a significant increase in risk of a pandemic but does not necessarily mean that a pandemic is a foregone conclusion.
Phase 5 is characterized by human-to-human spread of the virus into at least two countries in one WHO region. While most countries will not be affected at this stage, the declaration of Phase 5 is a strong signal that a pandemic is imminent and that the time to finalize the organization, communication, and implementation of the planned mitigation measures is short.
Phase 6, the pandemic phase, is characterized by community level outbreaks in at least one other country in a different WHO region in addition to the criteria defined in Phase 5. Designation of this phase will indicate that a global pandemic is under way.
During the post-peak period, pandemic disease levels in most countries with adequate surveillance will have dropped below peak observed levels. The post-peak period signifies that pandemic activity appears to be decreasing; however, it is uncertain if additional waves will occur and countries will need to be prepared for a second wave.
Previous pandemics have been characterized by waves of activity spread over months. Once the level of disease activity drops, a critical communications task will be to balance this information with the possibility of another wave. Pandemic waves can be separated by months and an immediate "at-ease" signal may be premature.
In the post-pandemic period, influenza disease activity will have returned to levels normally seen for seasonal influenza. It is expected that the pandemic virus will behave as a seasonal influenza A virus. At this stage, it is important to maintain surveillance and update pandemic preparedness and response plans accordingly. An intensive phase of recovery and evaluation may be required.
Government preparations for a potential H5N1 pandemic (2003-2009)
According to The New York Times as of March 2006, "governments worldwide have spent billions planning for a potential influenza pandemic: buying medicines, running disaster drills, [and] developing strategies for tighter border controls" due to the H5N1 threat.[93]
[T]he United States is collaborating closely with eight international organizations, including the World Health Organization (WHO), the Food and Agriculture Organization of the United Nations (FAO), the World Organization for Animal Health (OIE), and 88 foreign governments to address the situation through planning, greater monitoring, and full transparency in reporting and investigating avian influenza occurrences. The United States and these international partners have led global efforts to encourage countries to heighten surveillance for outbreaks in poultry and significant numbers of deaths in migratory birds and to rapidly introduce containment measures. The U.S. Agency for International Development (USAID) and the U.S. Departments of State, Health and Human Services (HHS), and Agriculture (USDA) are coordinating future international response measures on behalf of the White House with departments and agencies across the federal government.[94]
Together steps are being taken to "minimize the risk of further spread in animal populations", "reduce the risk of human infections", and "further support pandemic planning and preparedness".[94]
Ongoing detailed mutually coordinated onsite surveillance and analysis of human and animal H5N1 avian flu outbreaks are being conducted and reported by the USGS National Wildlife Health Center, the Centers for Disease Control and Prevention, the World Health Organization, the European Commission, the National Influenza Centers, and others.[95]
United Nations
In September 2005, David Nabarro, a lead UN health official warned that a bird flu outbreak could happen anytime and had the potential to kill 5–150 million people.[96]
World Health Organization
The World Health Organization (WHO), believing that the world was closer to another influenza pandemic than it has been any time since 1968, when the last of the 20th century's three pandemics swept the globe, has developed guidelines on pandemic influenza preparedness and response. The March 2005 plan includes guidance on roles and responsibilities in preparedness and response; information on pandemic phases; and recommended actions for before, during, and after a pandemic.[97]
United States
"[E]fforts by the federal government to prepare for pandemic influenza at the national level include a $100 million DHHS initiative in 2003 to build U.S. vaccine production. Several agencies within Department of Health and Human Services (DHHS) — including the Office of the Secretary, the Food and Drug Administration (FDA), CDC, and the National Institute of Allergy and Infectious Diseases (NIAID) — are in the process of working with vaccine manufacturers to facilitate production of pilot vaccine lots for both H5N1 and H9N2 strains as well as contracting for the manufacturing of 2 million doses of an H5N1 vaccine. This H5N1 vaccine production will provide a critical pilot test of the pandemic vaccine system; it will also be used for clinical trials to evaluate dose and immunogenicity and can provide initial vaccine for early use in the event of an emerging pandemic."[98]
Each State and Territory of the United States has a specific Pandemic Flu Plan which covers Avian Flu, Swine Flu (H1N1) and other potential influenza epidemics. The State Plans together with a professionally vetted search engine of flu related research, policies, and plans, is available at the current portal: Pandemic Flu Search.
On August 26, 2004, Secretary of Health and Human Services, Tommy Thompson released a draft Pandemic Influenza Response and Preparedness Plan,[99] which outlined a coordinated national strategy to prepare for and respond to an influenza pandemic. Public comments were accepted for 60 days.
In a speech before the United Nations General Assembly on September 14, 2005, President George W. Bush announced the creation of the International Partnership on Avian and Pandemic Influenza. The Partnership brings together nations and international organizations to improve global readiness by:
- elevating the issue on national agendas;
- coordinating efforts among donor and affected nations;
- mobilizing and leveraging resources;
- increasing transparency in disease reporting and surveillance; and
- building capacity to identify, contain and respond to a pandemic influenza.
On October 5, 2005, Democratic Senators Harry Reid, Evan Bayh, Dick Durbin, Ted Kennedy, Barack Obama, and Tom Harkin introduced the Pandemic Preparedness and Response Act as a proposal to deal with a possible outbreak.[100]
On October 27, 2005, the Department of Health and Human Services awarded a $62.5 million contract to Chiron Corporation to manufacture an avian influenza vaccine designed to protect against the H5N1 influenza virus strain. This followed a previous awarded $100 million contract to sanofi pasteur, the vaccines business of the sanofi-aventis Group, for avian flu vaccine.
In October 2005, President Bush urged bird flu vaccine manufacturers to increase their production.[101]
On November 1, 2005 President Bush unveiled the National Strategy To Safeguard Against The Danger of Pandemic Influenza.[102] He also submitted a request to Congress for $7.1 billion to begin implementing the plan. The request includes $251 million to detect and contain outbreaks before they spread around the world; $2.8 billion to accelerate development of cell-culture technology; $800 million for development of new treatments and vaccines; $1.519 billion for the Departments of Health and Human Services (HHS) and Defense to purchase influenza vaccines; $1.029 billion to stockpile antiviral medications; and $644 million to ensure that all levels of government are prepared to respond to a pandemic outbreak.[103]
On 6 March 2006, Mike Leavitt, Secretary of Health and Human Services, said U.S. health agencies are continuing to develop vaccine alternatives that will protect against the evolving avian influenza virus.[104]
The U.S. government, bracing for the possibility that migrating birds could carry a deadly strain of bird flu to North America, plans to test nearly eight times as many wild birds starting in April 2006 as have been tested in the past decade.[105]
On 8 March 2006, Dr. David Nabarro, senior U.N. coordinator for avian and human influenza, said that given the flight patterns of wild birds that have been spreading avian influenza (bird flu) from Asia to Europe and Africa, birds infected with the H5N1 virus could reach the Americas within the next six to 12 months.[106]
"Jul 5, 2006 (CIDRAP News) – In an update on pandemic influenza preparedness efforts, the federal government said last week it had stockpiled enough vaccine against H5N1 avian influenza virus to inoculate about 4 million people and enough antiviral medication to treat about 6.3 million."[107]
Canada
The Public Health Agency of Canada follows the WHO's categories, but has expanded them.[108] The Avian Flu scare of 2006 prompted The Canadian Public Health Agency to release an updated Pandemic Influenza Plan for Health Officials. This document was created to address the growing concern over the hazards faced by public health officials when exposed to sick or dying patients.
Malaysia
Since the Nipah virus outbreak in 1999, the Malaysian Health Ministry have put in place processes to be better prepared to protect the Malaysian population from the threat of infectious diseases. Malaysia was fully prepared during the Severe Acute Respiratory Syndrome (SARS) situation (Malaysia was not a SARS affected country) and the episode of the H5N1 (bird flu) outbreak in 2004.
The Malaysian government has developed a National Influenza Pandemic Preparedness Plan (NIPPP) which serves as a time bound guide for preparedness and response plan for influenza pandemic. It provides a policy and strategic framework for a multisectoral response and contains specific advice and actions to be undertaken by the Ministry of Health at the different levels, other governmental departments and agencies and non governmental organizations to ensure that resources are mobilized and used most efficiently before, during and after a pandemic episode.
See also
External resources
- The Great Pandemic: The United States in 1918
- PandemicFlu.gov
- Swine Flu News and Updates From Around the World
References
- List of epidemics — contains within it, influenza epidemics
- ↑ Nicholls H (February 2006). "Pandemic influenza: the inside story". PLoS Biology 4 (2): e50. doi:10.1371/journal.pbio.0040050. PMID 16464130. PMC 1363710. http://biology.plosjournals.org/archive/1545-7885/4/2/pdf/10.1371_journal.pbio.0040050-L.pdf. Retrieved 2009-11-03.
- ↑ Klenk et al. (2008). "Avian Influenza: Molecular Mechanisms of Pathogenesis and Host Range". Animal Viruses: Molecular Biology. Caister Academic Press. ISBN 978-1-904455-22-6. http://www.horizonpress.com/avir.
- ↑ Kawaoka Y (editor). (2006). Influenza Virology: Current Topics. Caister Academic Press. ISBN 978-1-904455-06-6 . ISBN 1904455069. http://www.horizonpress.com/flu.
- ↑ Current WHO phase of pandemic alert World Health Organization 2009
- ↑ World Health Organization. World now at the start of 2009 influenza pandemic. http://www.who.int/mediacentre/news/statements/2009/h1n1_pandemic_phase6_20090611/en/index.html.
- ↑ 6.0 6.1 Merck Manual Home Edition. "Influenza: Viral Infections". http://www.merck.com/mmhe/sec17/ch198/ch198c.html.
- ↑ Eccles, R (2005). "Understanding the symptoms of the common cold and influenza". The Lancet Infectious Diseases 5 (11): 718–25. doi:10.1016/S1473-3099(05)70270-X. PMID 16253889.
- ↑ Seasonal Flu vs. Stomach Flu by Kristina Duda, R.N.; accessed March 12, 2007 (Website: "About, Inc., A part of The New York Times Company")
- ↑ Suarez, DL; Spackman E, Senne DA, Bulaga L, Welsch AC, Froberg K (2003). "The effect of various disinfectants on detection of avian influenza virus by real time RT-PCR". Avian Diseases 47 (3 Suppl): 1091–5. doi:10.1637/0005-2086-47.s3.1091. PMID 14575118.
- ↑ Avian Influenza (Bird Flu): Implications for Human Disease. Physical characteristics of influenza A viruses. UMN CIDRAP.
- ↑ Flu viruses 'can live for decades' on ice, NZ Herald, November 30, 2006.
- ↑ "Avian influenza ("bird flu") fact sheet". World Health Organization. February 2006. http://www.who.int/mediacentre/factsheets/avian_influenza/en/. Retrieved 2006-10-20.
- ↑ "Influenza vaccines: WHO position paper". Weekly Epidemiological Record (WER). World Health Organization. 19 August 2005. pp. 277–88. http://www.who.int/wer/2005/wer8033.pdf.
- ↑ Villegas P (August 1998). [ps.fass.org/cgi/reprint/77/8/1143 "Viral diseases of the respiratory system"]. Poultry Science 77 (8): 1143–5. PMID 9706079. ps.fass.org/cgi/reprint/77/8/1143. Retrieved 2009-11-04.
- ↑ Horwood, F; Macfarlane J (2002). "Pneumococcal and influenza vaccination: current situation and future prospects" (PDF). Thorax 57 Suppl 2: II24–30. PMID 12364707. PMC 1766003. http://thorax.bmjjournals.com/cgi/reprint/57/suppl_2/ii24.pdf.
- ↑ Palese P (December 2004). "Influenza: old and new threats". Nature Medicine 10 (12 Suppl): S82–7. doi:10.1038/nm1141. PMID 15577936.
- ↑ See the articles for references that use these names.
- ↑ Harder, T. C. and Werner, O. (2006). "Avian Influenza". In Kamps, B. S., Hoffman, C. and Preiser, W. (ed.). Influenza Report 2006. Paris, France: Flying Publisher. ISBN 3-924774-51-X. http://www.influenzareport.com/ir/ai.htm. Retrieved 2006-04-18.
This e-book is under constant revision and is an excellent guide to Avian Influenza - ↑ CIDRAP - Center for Infectious Disease Research And Policy Pandemic Influenza Overview
- ↑ 20.0 20.1 Roos, Robert; Lisa Schnirring (February 1, 2007). "HHS ties pandemic mitigation advice to severity". University of Minnesota Center for Infectious Disease Research and Policy (CIDRAP). http://www.cidrap.umn.edu/cidrap/content/influenza/panflu/news/feb0107pandemic.html. Retrieved 2007-02-03.
- ↑ Barry, John M. (2005). "1 The Story of Influenza: 1918 Revisited: Lessons and Suggestions for Further Inquiry". In Knobler SL, Mack A, Mahmoud A, Lemon SM. The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. p. 62. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/62.html.
- ↑ Barry, John M. (2005). "1 The Story of Influenza: 1918 Revisited: Lessons and Suggestions for Further Inquiry". In Knobler SL, Mack A, Mahmoud A, Lemon SM. The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. p. 66. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/66.html.
- ↑ Barry, John M. (2005). "1 The Story of Influenza: 1918 Revisited: Lessons and Suggestions for Further Inquiry". In Knobler SL, Mack A, Mahmoud A, Lemon SM. The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. p. 59. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/59.html.
- ↑ 24.0 24.1 24.2 24.3 24.4 Barry, John M. (2005). "1 The Story of Influenza: 1918 Revisited: Lessons and Suggestions for Further Inquiry". The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. pp. 60–61. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/60.html.
- ↑ Barry, John M. (2005). "1 The Story of Influenza: 1918 Revisited: Lessons and Suggestions for Further Inquiry". In Knobler SL, Mack A, Mahmoud A, Lemon SM. The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. p. 63. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/63.html.
- ↑ Barry, John M. (2005). "1 The Story of Influenza: 1918 Revisited: Lessons and Suggestions for Further Inquiry". In Knobler SL, Mack A, Mahmoud A, Lemon SM. The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. p. 61. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/61.html.
- ↑ Hilleman M (Aug 19 2002). "Realities and enigmas of human viral influenza: pathogenesis, epidemiology and control". Vaccine 20 (25–26): 3068–87. doi:10.1016/S0264-410X(02)00254-2. PMID 12163258.
- ↑ 28.0 28.1 28.2 Taubenberger, Jeffery K.; Morens, David M. (January 2006). "1918 Influenza: the Mother of All Pandemics". Emerging Infectious Diseases (Centers for Disease Control and Prevention) 12 (1): 15–22. PMID 16494711. http://www.cdc.gov/ncidod/EID/vol12no01/05-0979.htm. Retrieved 2009-05-09.
- ↑ Andrew Price-Smith, Contagion and Chaos (Cambridge, MA: MIT Press,2009)
- ↑ 30.0 30.1 Patterson, KD; Pyle GF (Spring 1991). "The geography and mortality of the 1918 influenza pandemic". Bull Hist Med. 65 (1): 4–21. PMID 2021692.
- ↑ Potter, CW (October 2006). "A History of Influenza". J Appl Microbiol. 91 (4): 572–579. doi:10.1046/j.1365-2672.2001.01492.x. PMID 11576290. http://www.blackwell-synergy.com/doi/full/10.1046/j.1365-2672.2001.01492.x.
- ↑ "Historical Estimates of World Population". Census.gov. http://www.census.gov/ipc/www/worldhis.html. Retrieved 2008-11-03.
- ↑ Simonsen, L; Clarke M, Schonberger L, Arden N, Cox N, Fukuda K (July 1998). "Pandemic versus epidemic influenza mortality: a pattern of changing age distribution". J Infect Dis 178 (1): 53–60. PMID 9652423.
- ↑ http://www.actuaries.org.uk/__data/assets/pdf_file/0016/26026/0032-0054.pdf
- ↑ 35.0 35.1 Greene Jeffrey. Moline, Karen. [2006] (2006) The Bird Flu Pandemic. ISBN 0-312-36056-8.
- ↑ Goldsmith, Connie. [2007] (2007) Influenza: The Next Pandemic? 21st century publishing. ISBN 0-7613-9457-5
- ↑ 37.0 37.1 "Asia on high alert for flu virus". BBC News. 2009-04-27. http://news.bbc.co.uk/2/hi/americas/8019907.stm. Retrieved 2010-05-05.
- ↑ Paul, William E. (1993). Fundamental Immunology. New York: Plenum Press. pp. 1273. ISBN 0306444070. http://books.google.com/books?id=oPSG1PGmZUkC.
- ↑ "World health group issues alert Mexican president tries to isolate those with swine flu". Associated Press. April 25, 2009. http://www.jsonline.com/news/usandworld/43705182.html. Retrieved 2009-04-26.
- ↑ Mandel, Michael (April 26, 2009). "No need to panic ... yet Ontario officials are worried swine flu could be pandemic, killing thousands". Toronto Sun. http://www.torontosun.com/news/2009/04/26/9248411-sun.html. Retrieved 2009-04-26.
- ↑ U.S. Department of Health and Human Services, http://www.pandemicflu.gov/general/historicaloverview.html
- ↑ http://www.who.int/csr/don/2009_05_03/en/index.html
- ↑ "WHO: Swine flu pandemic has begun, 1st in 41 years". The Associated Press. June 11, 2009. http://www.google.com/hostednews/ap/article/ALeqM5jTkkEKE5LtPih_5Jcc-3MpD0gOYQD98OH0U00. Retrieved June 11, 2009.
- ↑ "Deadly new flu virus in U.S. and Mexico may go pandemic". New Scientist. April 28, 2009. Archived from the original on April 28, 2009. http://www.webcitation.org/5gNd9HTT9. Retrieved April 28, 2009.
- ↑ Pandemic (H1N1) 2009 - update 70, "As of 1 November 2009 [...] Laboratory-confirmed cases of the pandemic influenza H1N1 as officially reported to the WHO by States Parties to the International Health Regulations (2005)". Also see the WHO page [http://www.who.int/csr/disease/swineflu/updates/en/ Situation updates - Pandemic (H1N1) 2009, which has clickable links for all 70 updates, starting with the initial report of April 24, 2009.
- ↑ International Committee on Taxonomy of Viruses (2002). "46.0.1. Influenzavirus A". http://www.ncbi.nlm.nih.gov/ICTVdb/ICTVdB/46010000.htm. Retrieved 2006-04-17.
- ↑ Li KS, Guan Y, Wang J, Smith GJ, Xu KM, Duan L, Rahardjo AP, Puthavathana P, Buranathai C, Nguyen TD, Estoepangestie AT, Chaisingh A, Auewarakul P, Long HT, Hanh NT, Webby RJ, Poon LL, Chen H, Shortridge KF, Yuen KY, Webster RG, Peiris JS. (2004). "Genesis of a highly pathogenic and potentially pandemic H5N1 influenza virus in eastern Asia". Nature 430 (6996): 209–13. doi:10.1038/nature02746. PMID 15241415.
This was reprinted in 2005: Li, KS; Y. Guan, J. Wang, G.J.D. Smith et al., Y. Guan, J. Wang, G.J.D. Smith et al. (2005). "2 Today's Pandemic Threat: Genesis of a Highly Pathogenic and Potentially Pandemic H5N1 Influenza Virus in Eastern Asia". In Knobler SL, Mack A, Mahmoud A, Lemon SM. The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. pp. 116–130. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/116.html. - ↑ "Avian influenza strains are those well adapted to birds"EUROPEAN CENTRE FOR DISEASE PREVENTION AND CONTROL.
- ↑ Chapter Two : Avian Influenza by Timm C. Harder and Ortrud Werner from excellent free on-line Book called Influenza Report 2006 which is a medical textbook that provides a comprehensive overview of epidemic and pandemic influenza.
- ↑ Large-scale sequencing of human influenza reveals the dynamic nature of viral genome evolution Nature magazine presents a summary of what has been discovered in the Influenza Genome Sequencing Project.
- ↑ Beigel JH, Farrar J, Han AM, Hayden FG, Hyer R, de Jong MD, Lochindarat S, Nguyen TK, Nguyen TH, Tran TH, Nicoll A, Touch S, Yuen KY; Writing Committee of the World Health Organization (WHO) Consultation on Human Influenza A/H5 (September 29, 2005). "Avian influenza A (H5N1) infection in humans". N. Engl. J. Med. 353 (13): 1374–85. doi:10.1056/NEJMra052211. PMID 16192482. http://content.nejm.org/cgi/content/full/353/13/1374.
- ↑ "The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005)" Full text of online book by INSTITUTE OF MEDICINE OF THE NATIONAL ACADEMIES
- ↑ Here is the tree showing evolution by antigenic drift since 2002 that created dozens of highly pathogenic varieties of the Z genotype of avian flu virus H5N1, some of which are increasingly adapted to mammals.
- ↑ Evolutionary characterization of the six internal genes of H5N1 human influenza A virus
- ↑ Webster, R. G. and Walker, E. J. (2003). "The world is teetering on the edge of a pandemic that could kill a large fraction of the human population". American Scientist 91 (2): 122. doi:10.1511/2003.2.122. http://www.americanscientist.org/template/AssetDetail/assetid/17221?fulltext=true.
- ↑ United Nations (2005-09-29). "Press Conference by UN System Senior Coordinator for Avian, Human Influenza". UN News and Media Division, Department of Public Information, New York. http://www.un.org/News/briefings/docs/2005/050929_Nabarro.doc.htm. Retrieved 2006-04-17.
- ↑ Rosenthal, E. and Bradsher, K. (2006-03-16). "Is Business Ready for a Flu Pandemic?". The New York Times. http://www.nytimes.com/2006/03/16/business/16bird.html?_r=1&oref=slogin. Retrieved 2006-04-17.
- ↑ Science and Development Network article Pandemic flu: fighting an enemy that is yet to exist published May 3, 2006.
- ↑ Robert G. Webster, Ph.D., and Elena A. Govorkova, M.D., Ph.D. (November 23, 2006). "H5N1 Influenza — Continuing Evolution and Spread". NEJM 355 (21): 2174–2177. doi:10.1056/NEJMp068205. PMID 17124014. http://content.nejm.org/cgi/content/full/355/21/2174.
- ↑ CDC ARTICLE 1918 Influenza: the Mother of All Pandemics by Jeffery K. Taubenberger published January 2006
- ↑ Informaworld article Why is the world so poorly prepared for a pandemic of hypervirulent avian influenza? published December 2006
- ↑ CDC Key Facts About Avian Influenza (Bird Flu) and Avian Influenza A (H5N1) Virus
- ↑ Bloomberg News article Scientists Move Closer to Understanding Flu Virus Evolution published August 28, 2006
- ↑ Chen GW, Chang SC, Mok CK, et al. (September 2006). "Genomic signatures of human versus avian influenza A viruses". Emerging Infect. Dis. 12 (9): 1353–60. PMID 17073083. http://www.cdc.gov/ncidod/EID/vol12no09/06-0276.htm.
- ↑ de Jong MD, Bach VC, Phan TQ, Vo MH, Tran TT, Nguyen BH, Beld M, Le TP, Truong HK, Nguyen VV, Tran TH, Do QH, Farrar J (February 17, 2005). "Fatal avian influenza A (H5N1) in a child presenting with diarrhea followed by coma". N. Engl. J. Med. 352 (7): 686–91. doi:10.1056/NEJMoa044307. http://content.nejm.org/cgi/content/full/352/7/686. Retrieved 2009-11-03. PMID 15716562
- ↑ "The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005)" The National Academies Press, page 7
- ↑ Hazard in Hunt for New Flu: Looking for Bugs in All the Wrong Places The New York Times Published: November 8, 2005
- ↑ "WHO fears pandemic is 'imminent'". BBC News. 2009-04-30. http://news.bbc.co.uk/1/hi/world/americas/8025931.stm. Retrieved 2010-05-05.
- ↑ "WHO declares swine flu pandemic". BBC News. 2009-06-11. http://news.bbc.co.uk/1/hi/health/8094655.stm. Retrieved 2010-05-05.
- ↑ Detailed chart of its evolution here at PDF called Ecology and Evolution of the Flu
- ↑ "The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005)" The National Academies Press, page 115 - "There is particular pressure to recognize and heed the lessons of past influenza pandemics in the shadow of the worrisome 2003–2004 flu season. An early-onset, severe form of influenza A H3N2 made headlines when it claimed the lives of several children in the United States in late 2003. As a result, stronger than usual demand for annual flu inactivated vaccine outstripped the vaccine supply, of which 10 to 20 percent typically goes unused. Because statistics on pediatric flu deaths had not been collected previously, it is unknown if the 2003–2004 season witnessed a significant change in mortality patterns."
- ↑ Reason This Season's Flu Virus Is Resistant to 2 Standard Drugs By Altman LK, The New York Times, Published: January 15, 2006
- ↑ "The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005) " The National Academies Press, page 126
- ↑ 74.0 74.1 74.2 Council on Foreign Relations; Michael Osterholm, Rita Colwell, Laurie Garrett, Anthony S. Fauci, James F. Hoge, Nancy E. Roman (2005-06-16). "The Threat of Global Pandemics". Washington, DC: Council on Foreign Relations. http://www.cfr.org/pub8198/laurie_garrett_anthony_s_fauci_michael_osterholm_rita_colwell/the_threat_of_global_pandemics.php. Retrieved 2006-09-13.
- ↑ CDC
- ↑ World Health Organization. Pandemic influenza vaccine manufacturing process and timeline. http://www.who.int/csr/disease/swineflu/notes/h1n1_vaccine_20090806/en/.
- ↑ "Influenza vaccine manufacturers". World Health Organization. http://www.who.int/csr/disease/influenza/manulist/en/index.html. Retrieved 2006-09-13.
- ↑ "The clock is ticking". Phacilitate. http://www.phacilitate.co.uk/pages/phaciliate/article_fedson.html. Retrieved 2006-09-13.
- ↑ "Canada to launch avian flu vaccine trial". CTV.ca. 2005-04-20. http://www.ctv.ca/servlet/ArticleNews/story/CTVNews/1114000609146_109409809/. Retrieved 2006-09-13.
- ↑ [http://www.cidrap.umn.edu/cidrap/content/influenza/panflu/news/ jan2308gao.html "GAO cites barriers to antiviral, vaccine roles in pandemic"]. CIDRAP. http://www.cidrap.umn.edu/cidrap/content/influenza/panflu/news/ jan2308gao.html. Retrieved 2007-02-06.
- ↑ Zengerle P. U.S. to offer 10 pct of H1N1 vaccine internationally. September 17, 2009. http://www.reuters.com/article/healthNews/idUSTRE58G4MW20090917?feedType=RSS&feedName=healthNews.
- ↑ France to donate swine flu vaccines to WHO: presidency. September 17, 2009. http://www.france24.com/en/20090917-france-donate-swine-flu-vaccines-who-presidency.
- ↑ World Health Organization. Tables on the Clinical trials of pandemic influenza prototype vaccines. July 2009. http://www.who.int/vaccine_research/immunogenicity/immunogenicity_table.xls.
- ↑ US Food & Drug Administration. FDA Approves Vaccines for 2009 H1N1 Influenza Virus Approval Provides Important Tool to Fight Pandemic. September 15, 2009. http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm182399.htm.
- ↑ Wartime tactic doubles power of scarce bird-flu drug Nature 438, 6. 3 November 2005. doi:10.1038/438006a
- ↑ 86.0 86.1 86.2 "Pandemic (H1N1) 2009: frequently asked questions: What can I do?". World Health Organization. January 2010. http://www.who.int/csr/disease/swineflu/frequently_asked_questions/what/en/index.html. Retrieved 2010-02-28.
- ↑ "Stop Germs, Stay Healthy!". King County, Washington web site. http://www.metrokc.gov/health/stopgerms/index.htm. Retrieved 2006-09-13.
- ↑ "Non-pharmaceutical interventions: their role in reducing transmission and spread". World Health Organization. November 2006. http://www.who.int/csr/disease/avian_influenza/pharmaintervention2005_11_3/en/index.html. Retrieved 2006-09-13.
- ↑ Committee on Modeling Community Containment for Pandemic Influenza (11 Dec 2006). Modeling Community Containment for Pandemic Influenza: A Letter Report. The National Academies Press. pp. 47. ISBN 0-309-66819-0. http://www.iom.edu/?id=39066. Retrieved 6 May 2009.
- ↑ "WHO Pandemic Influenza Phases". Who.int. http://www.who.int/csr/disease/avian_influenza/phase/en/index.html. Retrieved 2009-04-27.
- ↑ The World Health Organization announces the current phase of the pandemic alert here. See "Assessing the pandemic threat" at [1]. The WHO published a first edition of the Global Influenza Preparedness Plan in 1999, and updated it in April 2005 and 2009.[2]. See [3] and [4] which define the responsibilities of the WHO and national authorities in case of an influenza pandemic. This is the first time a pandemic has been anticipated and is being prepared for. The aims of such plans are, broadly speaking, the following:
- Before a pandemic, attempt to prevent it and prepare for it in case prevention fails.
- If a pandemic does occur, to slow its spread and allow societies to function as normally as possible.
- ↑ "Current WHO phase of pandemic alert". WHO. http://www.who.int/csr/disease/avian_influenza/phase/en/.
- ↑ Rosenthal, Elisabeth; Bradsher, Keith (2006-03-16). "Is Business Ready for a Flu Pandemic?". The New York Times. http://www.nytimes.com/2006/03/16/business/16bird.html?_r=1&oref=slogin. Retrieved 2006-09-13.
- ↑ 94.0 94.1 "Avian Influenza Response: Key Actions to Date". USAID. http://www.usaid.gov/our_work/global_health/home/News/news_items/ai_activities.html. Retrieved 2006-09-16.
- ↑ "Monitoring Outbreaks". PandemicFlu.gov web site. http://www.pandemicflu.gov/outbreaks/. Retrieved 2006-09-16.
- ↑ "Bird flu 'could kill 150m people'". BBC News. 2005-09-30. http://news.bbc.co.uk/1/hi/world/asia-pacific/4292426.stm. Retrieved 2006-09-16.
- ↑ World Health Organization. Pandemic Influenza Preparedness and Response: A WHO Guidance Document. 2009. http://www.who.int/csr/disease/influenza/PIPGuidance09.pdf.
- ↑ Knobler SL, Mack A, Mahmoud A, Lemon SM, ed (2005). "Summary and Assessment". The Threat of Pandemic Influenza: Are We Ready? Workshop Summary (2005). The National Academies Press. p. 23. ISBN 0-309-09504-2. http://www.nap.edu/books/0309095042/html/23.html.
- ↑ "HHS Pandemic Influenza Plan". United States Department of Health and Human Services. 2006-03-20. http://www.hhs.gov/nvpo/pandemicplan/index.html.
- ↑ Senate Democratic Communications Center (2005-10-05). "Democrats Work to Protect Americans From Avian Flu". Press release. http://democrats.senate.gov/~dpc/press/05/2005A06424.html. Retrieved 2006-09-16.
- ↑ "Bush focuses on bird flu vaccines". BBC News. 2005-10-08. http://news.bbc.co.uk/1/hi/world/americas/4320678.stm. Retrieved 2006-09-16.
- ↑ "National Strategy for Pandemic Influenza". The White House. 2005-11-01. http://www.whitehouse.gov/homeland/pandemic-influenza.html. Retrieved 2006-09-16.
- ↑ "Bush Outlines $7 Billion Pandemic Flu Preparedness Plan". usinfo.state.gov web site. 2005-11-01. http://usinfo.state.gov/gi/Archive/2005/Nov/01-432345.html. Retrieved 2006-09-16.
- ↑ "U.S. Health Secretary Says More Bird Flu Vaccines Coming". usinfo.state.gov web site. 2006-03-07. http://usinfo.state.gov/gi/Archive/2006/Mar/07-312370.html. Retrieved 2006-09-16.
- ↑ Manning, Anita (2006-03-07). "With avian flu spreading, U.S. to expand its testing". USA Today. http://www.usatoday.com/tech/science/2006-03-07-bird-migration_x.htm. Retrieved 2006-09-16.
- ↑ Aita, Judy (2006-03-09). "United Nations Predicts Bird Flu in the Americas within a Year". usinfo.state.gov web site. http://usinfo.state.gov/gi/Archive/2006/Mar/09-520042.html?chanlid=globalissues. Retrieved 2006-09-16.
- ↑ "HHS has enough H5N1 vaccine for 4 million people". Center for Infectious Disease Research & Policy. 2006-07-05. http://www.cidrap.umn.edu/cidrap/content/influenza/panflu/news/jul0506hhsreport.html. article HHS has enough H5N1 vaccine for 4 million people published July 5, 2006
- ↑ "The Canadian Pandemic Influenza Plan for the Health Sector". Public Health Agency of Canada. http://www.phac-aspc.gc.ca/cpip-pclcpi/index-eng.php.
Will move this to Influenza but need to know if it's Cite or Cite Journal & is it hand Numbering ?
102. Notes 103 - 128 Reflect Some of the Earlier Research into Influenza by Dr L Hoyle who also published in cooperation with Springer Verlang The Influenza Viruses in 1968 103. Fractionation of the influenza virus with the object of producing subunit vaccine. Hoyle L, Barker SM. Postgrad Med J. 1973 Mar;49(569):193-4. 104. The nature of the toxic reaction of influenza virus towards lung tissue. Barker SM, Hoyle L. J Hyg (Lond). 1972 Sep;70(3):425-37 105. The chemical reactions of the haemagglutinins and neuraminidases of different strains of influenza viruses. 3. Effects of proteolytic enzymes. Hoyle L, Almeida JD. J Hyg (Lond). 1971 Sep;69(3):461-9. 106. The chemical reactions of the haemagglutinins and neuraminidases of different strains of influenza viruses. II. Effects of reagents modifying the higher order structure of the protein molecule. Hoyle L. J Hyg (Lond). 1969 Jun;67(2):301-10. 107. The chemical reactions of the haemagglutinins and neuraminidases of different strains of influenza viruses. I. Effect of reagents reacting with amino acids in the active centres. Hoyle L. J Hyg (Lond). 1969 Jun;67(2):289-99. 108. The chemical reactions of influenza virus proteins. Hoyle L, Hana L. J Pathol Bacteriol. 1966 Oct;92(2):447-60. 109. The structure and composition of the myxoviruses. III. The interaction of influenza virus particles with cytoplasmic particles derived from normal chorioallantoic membrane cells. HOYLE L, HORNE RW, WATERSON AP. Virology. 1962 Aug;17:533-42. 110. The entry of myxoviruses into the cell. HOYLE L. Cold Spring Harb Symp Quant Biol. 1962;27:113-21. 111. The structure and composition of the myxoviruses. II. Components released from the influenza virus particle by ether. HOYLE L, HORNE RW, WATERSON AP. Virology. 1961 Apr;13:448-59. 112. Amino acid composition of the protein components of influenza virus A. HOYLE L, DAVIES SP. Virology. 1961 Jan;13:53-7. 113. The use of influenza virus labelled with radio-sulphur in studies of the early stages of the interaction of virus with the host cell. HOYLE L, FINTER NB. J Hyg (Lond). 1957 Jun;55(2):290-7. 114. The nucleic acid and carbohydrate content of influenza virus A and of virus fractions produced by ether disintegration. FRISCH-NIGGEMEYER W, HOYLE L. J Hyg (Lond). 1956 Jun;54(2):201-12. 115. The disintegration of influenza virus particles on entry into the host cell; studies with virus labelled with radiophosphorus. HOYLE L, FRISCH-NIGGEMEYER W. J Hyg (Lond). 1955 Dec;53(4):474-86. 116. Release of influenza virus from the infected cell. HOYLE L. J Hyg (Lond). 1954 Jun;52(2):180-8. 117. The incorporation of radioactive phosphorus in the influenza virus and its distribution in serologically active virus fractions. HOYLE L, JOLLES B, MITCHELL RG. J Hyg (Lond). 1954 Mar;52(1):119-27. 118. Electron microscope studies of the structure of the influenza virus. HOYLE L, REED R, ASTBURY WT. Nature. 1953 Feb 7;171(4345):256-7. 119. Structure of the influenza virus; the relation between biological activity and chemical structure of virus fractions. HOYLE L. J Hyg (Lond). 1952 Jun;50(2):229-45. 120. The multiplication of complement-fixing antigen and red-cell agglutinin in the chorio- allantoic membrane of fertile eggs inoculated with influenza virus. HOYLE L. J Pathol Bacteriol. 1952 Apr;64(2):419-23. 121. Modern trends in the diagnosis and treatment of influenza. HOYLE L. Med Press. 1950 Nov 8;224(19):439-41. 122. Growth-cycle of influenza virus. HOYLE L. Nature. 1949 Dec 31;164(4183):1137. 123. The effect of triphenylmethane dyes on the intracellular growth of influenza virus A. HOYLE L. Br J Exp Pathol. 1949 Apr;30(2):123-9. 124. Difficulty experienced in the bacteriological diagnosis of paratyphoid fever in cases treated with sulphonamides. HOYLE L. Mon Bull Minist Health Public Health Lab Serv. 1949 Jan;8:22. 125. Influenza virus A; a study of the relations between virus, soluble antigen and host cell in fertile eggs inoculated with influenza virus. HOYLE L. Br J Exp Pathol. 1948 Oct;29(5):390-9. 126. Technique of the complement-fixation test in influenza. HOYLE L. Mon Bull Minist Health Public Health Lab Serv. 1948 May;7:114-6. 127. Diagnosis of epidemic influenza by the complement-fixation reaction. HOYLE L, FAIRBROTHER RW. Br Med J. 1947 Dec 20;2(4537):991-4. 128. ISOLATION OF THE INFLUENZA VIRUS AND THE RELATION OF ANTIBODIES TO INFECTION AND IMMUNITY THE MANCHESTER INFLUENZA EPIDEMIC OF 1937 LESLIE HOYLE, M.B., Ch.B.0 Royce Research Fellow AND R. W. FAIRBROTHER, D.Se., M.D., M.R.C.P.t MARCH 27, 1937 ISOLATION OF THE INFLUENZA VIRUS BMJ p655
External links
- Health-EU portal EU response to influenza
- [8] Award-winning book, "A Cruel Wind: Pandemic Flu in America, 1918-1920," by Dorothy A. Pettit, Ph.D. and Janice Bailie, Ph.D. (Timberlane Books, 2009)
- European Commission - Public Health EU coordination on Pandemic (H1N1) 2009
References
- Poland, G. A. (2006), "Vaccines against Avian Influenza—A Race against Time", N Eng J Med 354 (13): 1411–1413
- Treanor, J. J.; Campbell, J. D.; Zangwill, K. M.; Rowe, T.; Wolff, M. (2006), "Safety and Immunogenicity of an Inactivated Subvirion Influenza A (H5N1) Vaccine", N Eng J Med 354 (13): 1343–51
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
